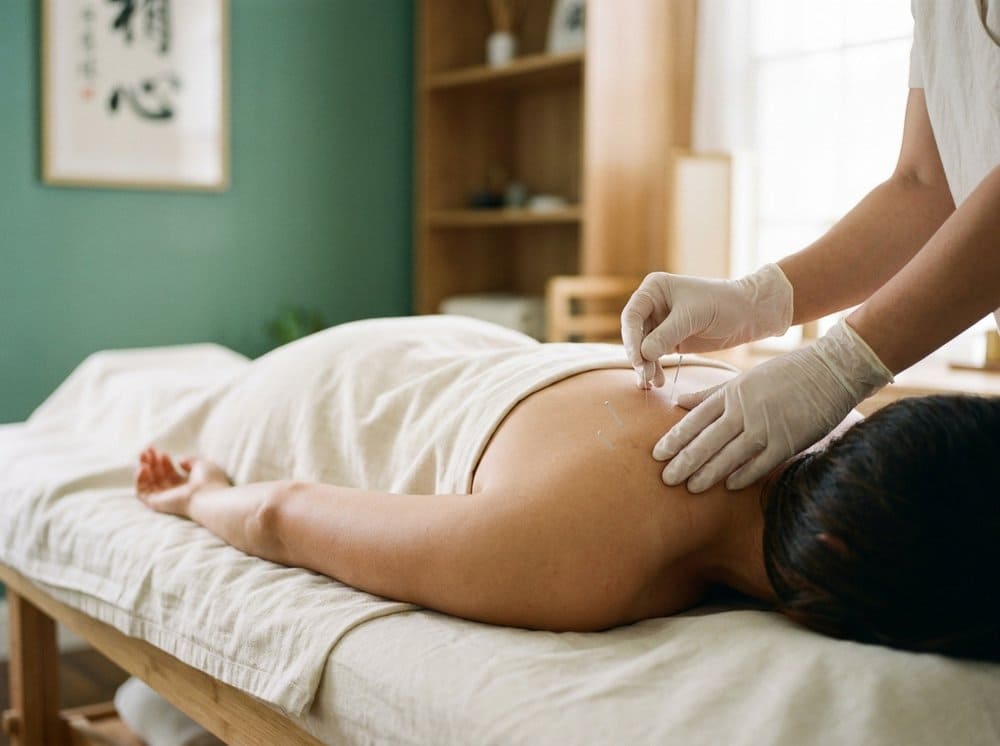
A question I am asked at almost every first consultation — usually late in the conversation, often with a hint of guilt — is some version of: "My physiotherapist said I should not do acupuncture. My friend said I should not do physio. Which one is right?" Neither is wrong. Both are speaking from real clinical experience of their respective disciplines. What neither tends to offer is a sober, patient-specific answer to the question of when each approach actually shines.
This note is that answer, as honestly as I can write it. I have practised acupuncture for more than twenty years. For the last three years I have co-managed a portion of my caseload with a physiotherapy group in Makati Medical Center. The clinical picture, once you have worked both sides, is far less adversarial than internet forums suggest.
What each modality actually does
It helps to begin with what is, and is not, inside each scope.
Acupuncture, properly practised, is a neurological and vascular intervention. Fine needles stimulate peripheral nerves, modulate central pain processing through well-documented endogenous opioid and serotonergic pathways, increase local microcirculation, and reduce inflammatory cytokine activity in the needled tissue. The classical zhen jiu framework describes this in the language of qi, channel, and meridian, but the modern mechanism is not mysterious. It is well within mainstream physiology. Our service page on acupuncture lays out the conditions we treat most often.
Physiotherapy, properly practised, is a movement-restoration and progressive-loading intervention. Through assessment, manual therapy, and — critically — graded exercise, the physio rebuilds the capacity of muscle, tendon, and joint to tolerate load. This is the only discipline that reliably produces long-term hypertrophy and tendon remodelling. Needles cannot do that. Neither can herbs.
They address different parts of the same problem. In most chronic joint presentations, both parts need attention.
Where acupuncture wins
- Acute pain crisis, where the patient cannot yet move through the exercises the physio wants to prescribe. Needles can bring a pain score from seven-out-of-ten to three-out-of-ten in a single forty-five-minute session. That often unlocks the rehabilitation programme that has been stalled for weeks.
- Chronic regional pain syndromes with strong neuropathic components — burning pain, shooting electrical sensations, sleep-disrupting ache that does not respond to any exercise protocol. Acupuncture's effect on central sensitisation is, in my clinical experience, its strongest indication.
- Pattern-level interventions — the whole-body imbalances that the classical bi-syndrome framework captures and Western reductive diagnosis often misses. The patient whose knee hurts because their spleen qi is depleted and dampness has accumulated in the lower limb does not, primarily, need a stronger quadriceps. They need the damp cleared. This diagnostic reading is covered at length in our piece on how TCM reads chronic joint pain.
- Climatic or seasonal flares, where a barometric-pressure-mediated swelling needs to be drained quickly. A single acupuncture-plus-cupping session in the first twenty-four hours of a storm-triggered flare is, in my experience, faster than any exercise-based alternative.
Where physiotherapy wins
- Post-surgical rehabilitation. After a meniscal repair, ACL reconstruction, or total knee replacement, the progressive loading schedule a physio builds is irreplaceable. Acupuncture can complement the process — pain relief, anti-inflammatory support — but it cannot substitute for the tendon-and-muscle-rebuilding work.
- Biomechanical dysfunction. A patient whose knee pain is driven by a weak gluteus medius, a tight iliotibial band, and a pronated foot needs, above all, to strengthen the glute and retrain the movement pattern. Needles will quiet the symptom. Only loaded exercise will fix the cause.
- Sport-specific return-to-play. The graduated plyometric and neuromuscular retraining that a sports physio delivers cannot be replicated in an acupuncture clinic.
- Young, deconditioned patients. A thirty-year-old with new-onset back pain from a desk job needs, more than anything, to move. Passive modalities — needles, massage, heat — can feel excellent in the moment but often delay the active work that matters.
Where both are needed
The majority of chronic joint pain cases sit here. The pattern is the same in most of my shared-care patients: acupuncture (and often tuina massage) to reduce pain and release soft-tissue restrictions enough that the physio's exercise programme becomes tolerable, and physiotherapy to rebuild the structural capacity that keeps the pain from returning. When the two are sequenced well — often, in practice, alternating days in the same week — patients improve on a clearly steeper curve than either modality produces alone.
"Needles open the door. Exercise walks the patient through it. Take either away and the house remains closed." — a line I have used so often with patients it has become my standard explanation.
A three-column clinical comparison
For patients who want a quick decision-aid, here is the short version I give most often.
- Acute inflammatory flare / central pain / seasonal weather-triggered pain — start with acupuncture, add physio after two to four weeks once movement is tolerable.
- Post-surgical / biomechanical / young-deconditioned — start with physio, add acupuncture as needed for breakthrough pain or sleep-disturbing symptoms.
- Chronic mixed osteoarthritis with climate sensitivity, stiffness, and low-level daily pain — combine from the start. Acupuncture weekly for four to six weeks, alongside a physio-prescribed exercise programme of twenty minutes daily. This is the most common presentation in our Makati caseload, and the combined approach is what I recommend for it.
What good cross-referral looks like
A good acupuncturist refers out to a physio when they see a case whose primary driver is biomechanical. A good physio refers in for acupuncture when pain is preventing exercise progression. Both communicate directly where possible — a short message between practitioners is worth a week of guessing. In Makati, our clinic maintains working relationships with several physiotherapy groups, and the results for shared patients are consistently better than what either of us produces alone. For a deeper view of how we integrate modalities in our own clinic, see our eastern wisdom note on integrative practice.
What a bad answer looks like
A bad answer comes from a practitioner — of either discipline — who insists their modality can do everything. It usually cannot. The honest clinician knows the edges of their tools. If your physiotherapist has never referred a patient for acupuncture, or your acupuncturist has never referred a patient for physiotherapy, that is a useful piece of information.
A closing note
The adversarial framing that sometimes surrounds this question serves no patient. Both modalities have real evidence bases, real limitations, and real indications. A careful clinician, in either discipline, should be able to tell you when the tools they hold are the right ones — and when the patient would be better served walking across the hall. That is the practice I try to run, and it is the standard I encourage patients to hold any clinician, TCM or Western, accountable to.